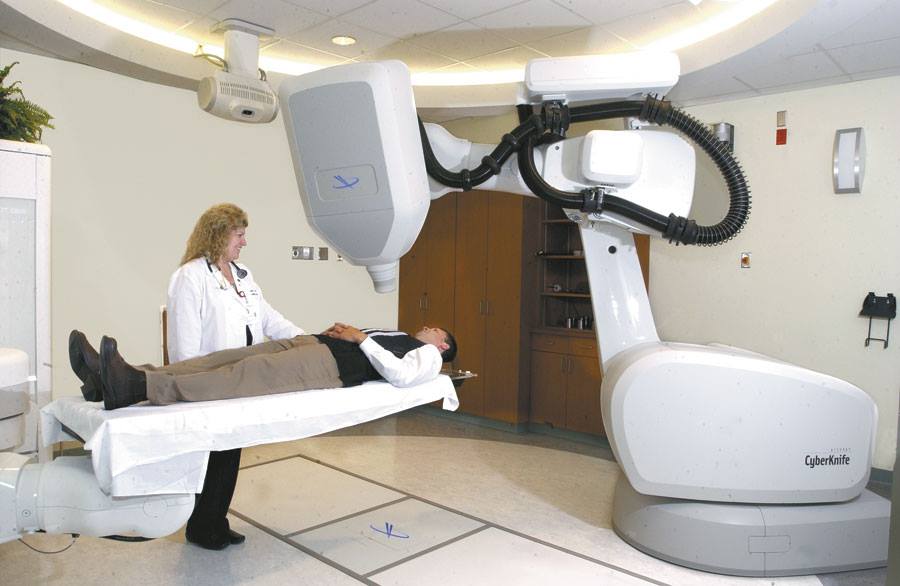
A New Study Confirms the Effectiveness & Safety of CyberKnife Radiation Therapy for Oligometastatic Cancer published in JAMA Oncology.
Radiation Oncologist Dr. Mark Pomper explains in the simplest way why CyberKnife is an excellent treatment option.
Here’s the Study & the Results:
Safety and Survival Rates Associated With Ablative Stereotactic Radiotherapy for Patients With Oligometastatic Cancer A Systematic Review and Meta-analysis
Key Points: Question
Is stereotactic ablative radiotherapy safe and clinically beneficial in the management of oligometastatic cancer?
Findings This meta-analysis of 21 trials comprising 943 patients and 1290 oligometastases found that stereotactic ablative radiotherapy was associated with rates of clinically significant acute and late toxic effects of less than 13% and with clinically acceptable rates of 1-year local control overall survival, and progression-free survival.
These findings were noted among a heterogeneous group of patients treated in prospective trials.
Meaning
The findings of this study suggest that stereotactic ablative radiotherapy is generally safe and well tolerated in the oligometastatic setting and remains a viable treatment option in appropriately selected patients; further study addressing sources of heterogeneity is warranted.
Importance The oligometastatic paradigm postulates that patients with a limited number of metastases can be treated with ablative local therapy to each site of disease with curative intent.
Stereotactic ablative radiotherapy (SABR) is a radiation technique that has become widely used in this setting. However, prospective data are limited and are mainly from single institutional studies.
Objective
To conduct a meta-analysis to characterize the safety and clinical benefit of SABR in oligometastatic cancer.
Data Sources
A comprehensive search was conducted in PubMed/MEDLINE, Embase, Cochrane Database of Systematic Reviews, and Cumulative Index to Nursing and Allied Health Literature on December 23, 2019, that included prospective clinical trials and review articles that were published within the past 15 years.
Study Selection
Inclusion criteria were single-arm or multiarm prospective trials including patients with oligometastatic cancer (ie, ≤5 sites of extracranial disease), and SABR was administered in less than or equal to 8 fractions with greater than or equal to 5 Gy/fraction.
Data Extraction and Synthesis
The Population, Intervention, Control, Outcomes and Study Design; Preferred Reporting Items for Systematic Reviews and Meta-analyses; and Meta-analysis of Observational Studies in Epidemiology methods were used to identify eligible studies. Study eligibility and data extraction were reviewed by 3 authors independently. Random-effects meta-analyses using the Knapp-Hartung correction, arcsine transformation, and restricted maximum likelihood method were conducted. Main Outcomes and Measures Safety (acute and late grade 3-5 toxic effects) and clinical benefit (1-year local control, 1-year overall survival, and 1-year progression-free survival).
Results Twenty-one studies comprising 943 patients and 1290 oligometastases were included. Median age was 63.8 years (interquartile range, 59.6-66.1 years) and median follow-up was 16.9 months (interquartile range, 13.7-24.5 months). The most common primary sites were prostate (22.9%), colorectal (16.6%), breast (13.1%), and lung (12.8%). The estimate for acute grade 3 to 5 toxic effect rates under the random-effects models was 1.2% (95% CI, 0%-3.8%; I2 = 50%; 95% CI, 3%-74%; and τ = 0.20%; 95% CI, 0.00%-1.43%), and the estimate for late grade 3 to 5 toxic effects was 1.7% (95% CI, 0.2%-4.6%; I2 = 54%; 95% CI, 11%-76%; and τ = 0.25%; 0.01%-1.00%). The random-effects estimate for 1-year local control was 94.7% (95% CI, 88.6%-98.6%; I2 = 90%; 95% CI, 86%-94%; and τ = 0.81%; 95% CI, 0.36%-2.38%]). The estimate for 1-year overall survival was 85.4% (95% CI, 77.1%-92.0%; I2 = 82%; 95% CI, 71%-88%; and τ = 0.72%; 95% CI, 0.30%-2.09%) and 51.4% (95% CI, 42.7%-60.1%; I2 = 58%; 95% CI, 17%-78%; and τ = 0.20%; 95% CI, 0.02%-1.21%) for 1-year progression-free survival.
Conclusions and Relevance
In this meta-analysis, SABR appears to be relatively safe in patients with oligometastatic cancer with clinically acceptable rates of acute and late grade 3 to 5 toxic effects less than 13% and with clinically acceptable rates of 1-year local control overall survival, and progression-free survival. These findings are hypothesis generating and require validation by ongoing and planned prospective clinical trials. Call the CyberKnife Center Miami if we can help you or a loved one with oligometastatic cancer or any kind of cancer. We are happy to answer all your questions 305-279-2900. And go to our website now to find out more about CyberKnife, what we treat and how. www.cyberknifemiami.com